Help for IBS
Do you suffer from Irritable Bowel Syndrome (IBS) and feel like your current diet is making things worse? Current research indicates that fermentable oligosaccharides, disaccharides, monosaccharides, and polyols, or FODMAPs, may increase symptoms such as gas, bloating, abdominal pain, diarrhea, and other symptoms associated with IBS. FODMAPs are types of short-chain, poorly absorbed, and rapidly fermentable carbohydrates. It is understandable if you haven’t heard of FODMAPs until now, since the low-FODMAP diet is just beginning to gain the recognition it deserves in the U.S. It was originally researched and implemented in Australia by Dr. Sue Shepherd in 1999. Shepherd identified that some people poorly absorb these types of carbohydrates, and when they eventually reach the large intestine, those carbohydrates are the perfect food for the bacteria that resides there. Once the bacteria digest the carbohydrate, they produce gas and pull water into the large intestine, which contributes to the painful symptoms associated with IBS.
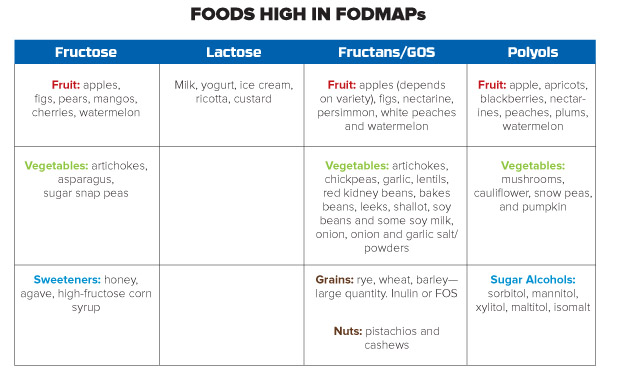
FODMAPs are found in foods we eat everyday. The chart from Kate Scarlata, R.D., a nationally known digestive expert, contains examples of foods high in FODMAPs. You can find a more detailed list of low FODMAP foods as well as recipes and grocery shopping tips on Scarlata’s website, “Well balanced. Food. Life. Travel.” (blog.katescarlata.com)
Diet Basics
The premise behind using a low-FODMAP diet to help manage IBS is that each person has a certain tolerance level for the total amount of FODMAPs consumed in a day. For example: One person may be able to eat a large apple, several cups of spinach, and a bowl of ice cream with little or no issues, whereas that same amount and type of food may exacerbate IBS symptoms in someone else. Finding your threshold for high FODMAP foods is important, and by following the two-phase FODMAP diet, you will be able to identify this limit.
Prior to starting the diet, keep a record of your IBS symptoms. Doing so allows you to objectively look back at the data during the diet to determine whether you have had a reduction in symptoms. The diet works in two phases. During the initial phase, foods high in FODMAPs are eliminated for at least two weeks. At the end of the trial phase, compare the symptoms you experienced prior to starting the diet to those you are experiencing now; do you see a difference? If so, start the second phase. In this phase, you will introduce foods high in FODMAPs, one food group at a time, back into your diet. The goal is to identify which foods cause a flare up in symptoms and determine a tolerance level for certain types of FODMAPs. For example: You love high-fructose foods such as fruits and vegetables, so you start with that group, slowly adding in those foods while noting any increase in IBS symptoms. Remember that it’s the total amount of FODMAPs consumed over a day that has the greatest impact on your gastrointestinal function, not just one meal or snack. Once all the food groups have been tested, you will be able to determine your tolerance for foods high in FODMAPs as well as your threshold level by analyzing the results and looking at where your symptoms increased and decreased. Although you may still experience some IBS symptoms at the conclusion of the diet, the goal behind monitoring FODMAPs is to greatly reduce symptoms while maintaining a healthy diet.
New research on FODMAPs is being published and updated foods lists are available periodically. Discrepancies can exist between FODMAP food lists, so check the print date to determine the most current one. Since FODMAP diets can be tricky to start, a registered dietitian’s assistance is essential and there are several of us in the Austin area who can help. I also highly recommend the following print and Web resources: “IBS—Free At Last!” by Patsy Catsos, M.S., R.D., L.D.; Monash University (med.monash.edu.au); and, as mentioned previously, Kate Scarlata’s blog (blog.katescarlata.com).